Patient Presentation
A 31-year-old man presented with an irreducible protruding anal mass accompanied by recurrent bright red rectal bleeding. He worked as a laborer and reported constipation with stools, frequent straining, and defecation deferral. The mass was initially intermittent during defecation but progressively enlarged and became irreducible. He reported anal irritation while sitting and defecation without sharp pain. The patient denied fecal or flatus incontinence, melena, weight loss, or systemic symptoms.
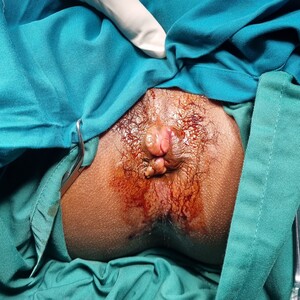
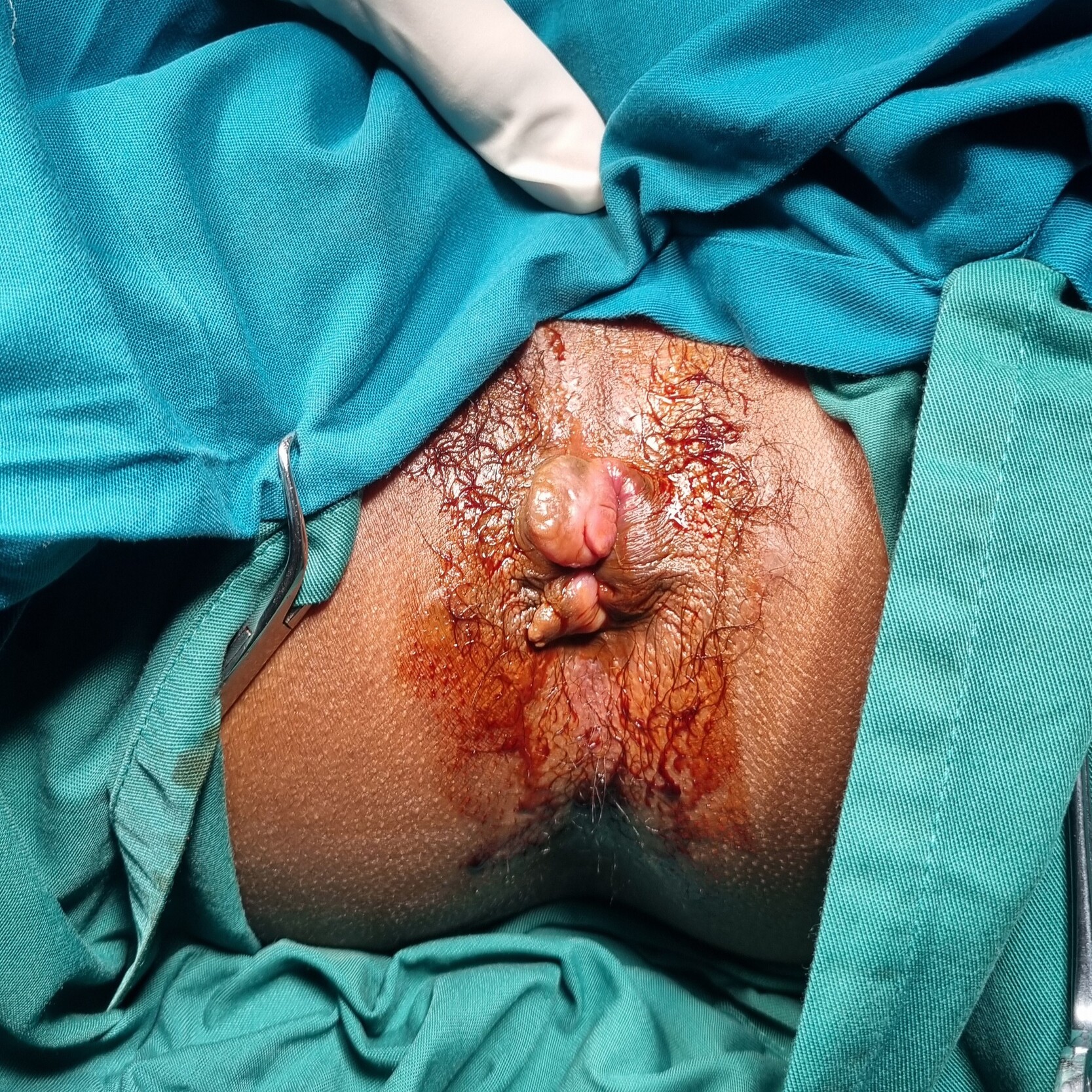
Physical examination, performed with the patient in the left lateral position, revealed a lobulated segmental mucosal mass protruding from the anal canal, consistent with prolapsed internal hemorrhoids (Figure 1). The exposed mucosa appeared edematous, without thrombosis or necrosis, and manual reduction was attempted, but was unsuccessful. Digital rectal examination was limited by discomfort, preserved sphincter contraction, and the absence of a palpable intrarectal mass. Anoscopy confirmed an enlarged internal haemorrhoidal cushion. Laboratory evaluation revealed microcytic hypochromic anemia (hemoglobin, 11.6 g/dL; mean corpuscular volume, 66.4 fL). Taken together, irreducible prolapse, segmental mucosal morphology, recurrent distal rectal bleeding, and associated anemia supported the decision to proceed with definitive surgical management.
Diagnosis
Grade IV internal hemorrhoidal disease (irreducible prolapse).
Discussion
Grade IV internal hemorrhoidal disease is characterized by permanently irreducible prolapse due to pathological enlargement and distal displacement of the anal vascular cushions, with recurrent bleeding and functional impairment often requiring surgery.1 Internal hemorrhoids usually cause painless bright red rectal bleeding, but fixed prolapse may result in local discomfort from mucosal edema and inflammation rather than sharp pain.2
Diagnosis was primarily clinical. When evaluating a protruding anal mass, the differential diagnoses include full-thickness rectal prolapse, thrombosed external hemorrhoids, mucosal prolapse syndrome, and anorectal neoplasms. Full-thickness rectal prolapse shows concentric circumferential folds, whereas prolapsed internal hemorrhoids show segmental folds.3 Thrombosed external hemorrhoids cause acute pain. Mucosal prolapse syndrome is linked to chronic straining and ulceration, and anal neoplasms present as irregular, indurated, non-reducible masses with persistent bleeding.4 In this case, the segmental morphology, absence of acute pain, and anoscopic confirmation of enlarged internal hemorrhoidal cushions supported grade IV internal hemorrhoidal disease.
Bright red rectal bleeding accompanied by anemia warrants careful evaluation to prevent premature diagnostic closure.5 Although hemorrhoids are a common benign source of distal bleeding, microcytic anemia suggests clinically significant chronic blood loss. The absence of blood mixed with stool supports a distal anorectal source but does not exclude alternative gastrointestinal pathology; further evaluation should be guided by age, risk factors, and alarm features.
Given the irreducible grade IV prolapse associated with anemia and functional impairment, operative management was favored over conservative or office-based interventions. Excisional hemorrhoidectomy was selected as the definitive treatment because of limited efficacy of nonoperative techniques in advanced disease and its durable control of bleeding and prolapse.1,5
Ethics approval
Written informed consent was obtained from the patient for the publication of this clinical image study.
Availability of data and material
Data sharing is not applicable to this article as no new data were created or analyzed in this study.
Competing interests
The authors declare no known competing financial interests or personal relationships that could have influenced the work reported in this paper.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Authors Contributions
II conceptualized the study and drafted the manuscript. MRDS contributed to manuscript drafting and critical revision. AHR supervised the study and provided validation and resources. All authors reviewed and approved the final manuscript.
Acknowledgement
None.