Introduction
The acute scrotum is a diagnostic conundrum in urological practice that needs to be managed in a timely manner because conditions like testicular torsion and Fournier’s gangrene involve surgical emergencies. Though most clinicians are well aware of infectious and torsional causes for an acutely swollen scrotum, scrotal and penile oedema as a complication of systemic diseases often goes unrecognized, which might lead to unnecessary surgical exploration or delay in the treatment of the predisposing condition itself.1
Generalized fluid accumulation in the interstitial space defines anasarca, a condition which often presents with dependent regions such as the lower extremities in any gender and, in males, also with marked scrotal wall and penis swelling.2 This pathophysiological process is due to disturbance in Starling forces that govern fluid movement between vascular and interstitial compartments. Common systemic causes include congestive heart failure, nephrotic syndrome, liver cirrhosis, and severe hypoalbuminemia from various causes.3
In males with advanced systemic fluid overload, the scrotal wall and penis are one of the more significant sites of edema accumulation due to their dependent position and loose subcutaneous tissue.4 This can lead to marked enlargement causing considerable discomfort, impaired ambulation, and urinary difficulties. When these patients are admitted through the emergency departments, the dramatic appearance of genital swelling often prompts urgent urological consultation to exclude acute surgical pathology.2
We illustrate two cases demonstrating this clinical scenario: a patient with decompensated heart failure with massive scrotal and penile oedema and another with nephrotic syndrome developing significant scrotal oedema. These case examples emphasize the importance of recognizing systemic causes of genital swelling and the role of clinical assessment and imaging to obviate unnecessary surgical interventions.
Case Presentations
Case 1: Massive Scrotal and Penile Edema Secondary to Decompensated Heart Failure
A 68-year-old male with a 15-year history of ischemic cardiomyopathy presented to the emergency department with progressive bilateral scrotal and penile swelling over the preceding 72 hours. His cardiac history included two previous myocardial infarctions, an ejection fraction of 20% on recent echocardiography, and multiple hospitalizations for acute heart failure exacerbations in the past year . His medication regimen included maximum doses of ACE inhibitors, beta-blockers, spironolactone, and loop diuretics.
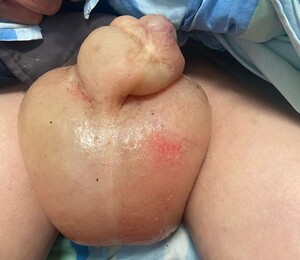
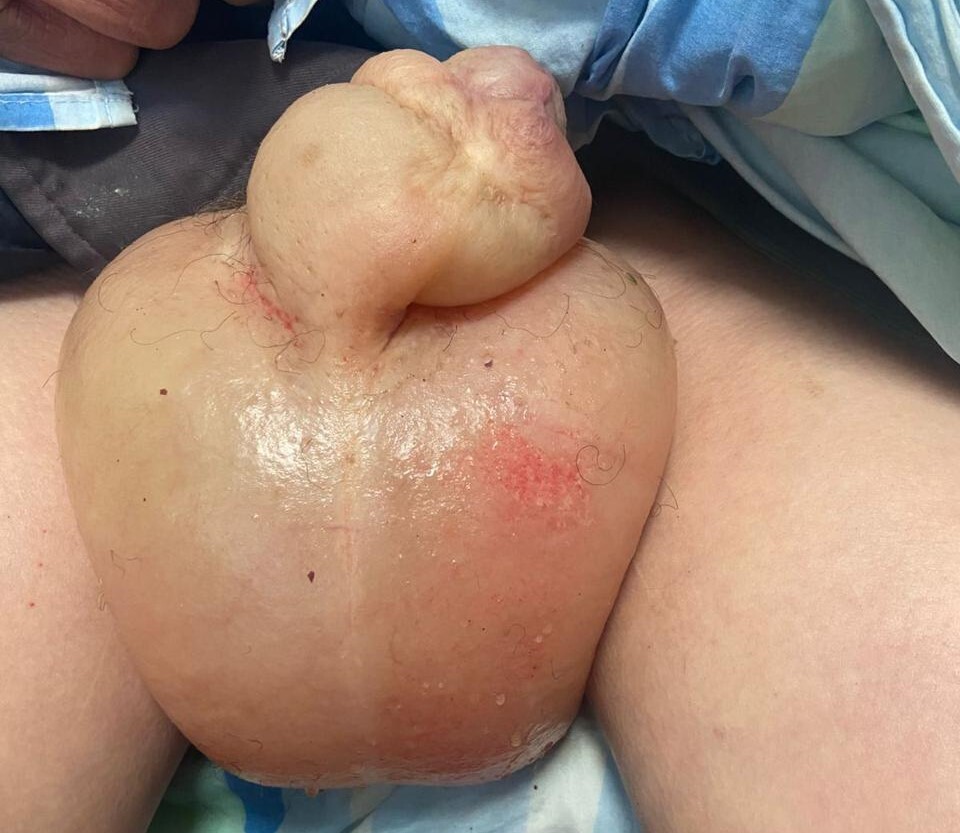
The patient reported that the scrotal and penile swelling had developed rapidly, accompanied by marked discomfort and difficulty with ambulation and urination. He denied scrotal pain, fever, trauma, or urinary symptoms suggestive of infection. Physical examination revealed significant generalized anasarca with bilateral pitting edema of the lower extremities extending to the sacral region . The scrotum was markedly enlarged, tense, and edematous with stretched, shiny skin. The penis was also significantly swollen, with the edema extending from the penile shaft to involve the prepuce. The genital skin appeared erythematous due to tension but without signs of crepitus, purulent discharge, or necrosis. Both testes were palpable within the edematous scrotum, of normal consistency and non-tender. There was no inguinal lymphadenopathy.(Figure 1)
Vital signs showed tachycardia (heart rate 102 bpm) and mild tachypnea (respiratory rate 22/min). Laboratory investigations revealed mild leukocytosis (11,000/μL), hyponatremia (sodium 128 mmol/L), elevated BNP (2,450 pg/mL), and mild renal impairment (creatinine 1.8 mg/dL) consistent with cardiorenal syndrome . The urology service was consulted urgently to exclude Fournier’s gangrene or testicular torsion.
Scrotal ultrasound examination was conducted bedside by the consultant urologist. There was thickening of the scrotal wall and diffuse subcutaneous edema. Both testes had homogeneous parenchyma with intact echogenicity. There were no focal lesions or fluid collections. There was no air in the scrotal subcutaneous tissue or evidence suggesting testicular torsion. There was no clinical evidence of acute surgical features.
Formal risk stratification tools such as the TWIST score (Testicular Workup for Ischemia and Suspected Torsion) were not applied, as the clinical presentation—bilateral symmetric involvement, absence of testicular pain or tenderness, palpable non-tender testes, and presence of severe generalized anasarca in a patient with known decompensated heart failure—made testicular torsion highly unlikely from clinical assessment alone.
The patient was admitted under cardiology care for optimization of heart failure management . Due to electrolyte imbalances and concerns about further deteriorating renal function, aggressive diuresis was not immediately feasible. Conservative management included scrotal and penile elevation, supportive garments, and careful fluid balance monitoring . Over the following five days, with gradual improvement in cardiac function and cautious diuretic adjustment, the scrotal and penile edema progressively decreased. By discharge, the genital swelling had reduced by approximately 70%, and the patient reported significant improvement in comfort and mobility.
Case 2: Scrotal Edema Secondary to Nephrotic Syndrome
A 42-year-old male with recently diagnosed nephrotic syndrome presented with progressive scrotal and lower extremity edema over two weeks. He had been diagnosed three months earlier following workup for peripheral edema and proteinuria. Renal biopsy revealed focal segmental glomerulosclerosis (FSGS). His initial presentation included severe proteinuria (24-hour urine protein 8.5 g), hypoalbuminemia (serum albumin 2.1 g/dL), and hyperlipidemia . He had been started on high-dose corticosteroids, ACE inhibitors, and diuretics, with partial initial response.
However, two weeks prior to this presentation, he experienced a relapse with worsening proteinuria and progressive edema . The scrotal swelling had become particularly distressing, causing difficulty with walking, sitting comfortably, and urination. He denied fever, scrotal pain, or urinary symptoms. His wife had noted the rapid progression of the swelling and insisted on emergency evaluation, concerned about possible infection.
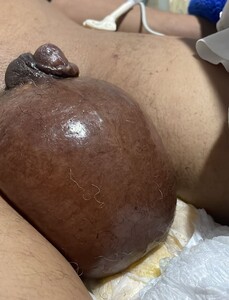
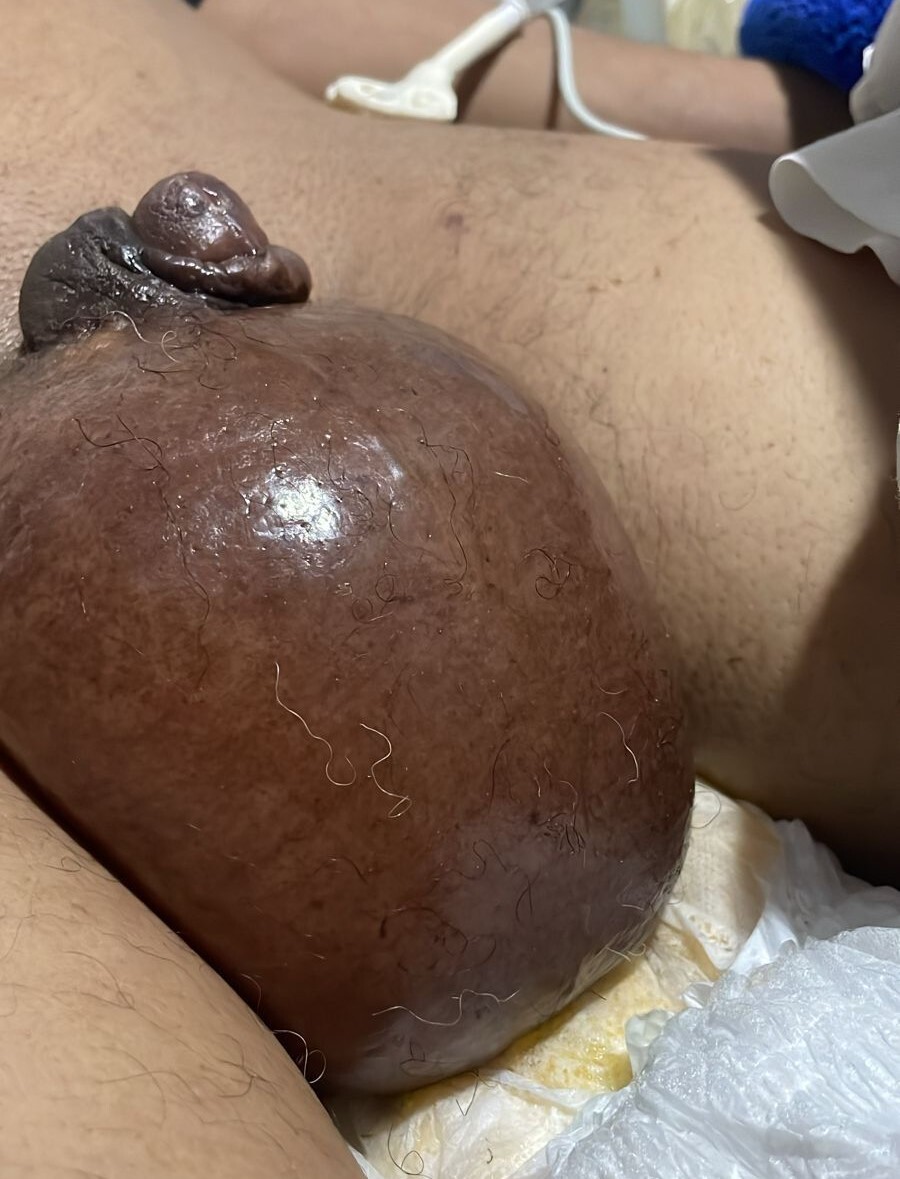
Physical examination revealed a well-appearing patient with marked generalized edema . The scrotum was significantly enlarged, approximately four times normal size, with taut, translucent skin showing prominent superficial vessels. The scrotal skin was warm but not hot, with no crepitus, purulent drainage, or areas of necrosis. Both testes were palpable, non-tender, and of normal consistency. Bilateral pitting edema extended from the feet to the mid-thighs. There was no abdominal distension or ascites.(Figure 2)
Laboratory findings showed severe hypoalbuminemia (1.8 g/dL), massive proteinuria (urine protein/creatinine ratio 9.2), normal white blood cell count (7,500/μL), and preserved renal function (creatinine 1.1 mg/dL) . Urgent urology consultation was requested to evaluate for possible Fournier’s gangrene or other acute scrotal pathology.
Point-of-care scrotal ultrasound examination was done by the urology consultant. There was noticeable thickness of the scrotal wall with a large amount of subcutaneous fluid accumulation. However, the testes had normal size, uniform echo texture, and no signs of masses, fluid, or inflammation. Based on the ultrasound and the clinical presentation, scrotal edema due to systemic hypoalbuminemia was present without needing surgical correction.
Given the bilateral nature of the swelling, absence of testicular tenderness, and clear systemic cause (severe nephrotic syndrome with marked hypoalbuminemia), formal clinical scoring for testicular torsion was deemed unnecessary.
The patient was admitted for intensive medical management of nephrotic syndrome . Treatment included intravenous albumin infusion followed by aggressive diuresis with furosemide, strict sodium restriction, and continuation of immunosuppressive therapy . Scrotal elevation and supportive measures provided symptomatic relief . Over seven days of hospitalization, there was gradual reduction in scrotal edema. The patient experienced significant symptomatic improvement and was discharged with outpatient nephrology follow-up. At two-week follow-up, the scrotal edema had nearly completely resolved, and his quality of life had markedly improved.
Discussion
These two cases illustrate an important but often overlooked cause of scrotal and penile swelling: secondary edema from systemic diseases causing fluid overload. While the acute scrotum typically prompts immediate consideration of surgical emergencies such as testicular torsion, epididymo-orchitis, or Fournier’s gangrene, systemic causes of genital edema should be recognized, particularly in patients with known cardiac, renal, or hepatic disease.1,4
Pathophysiology of Scrotal and Penile Edema in Systemic Disease
Scrotal and penile edema in the setting of systemic diseases results from disturbances in Starling forces that regulate fluid movement across capillary membranes . In heart failure, the increased venous pressure elevates capillary hydrostatic pressure and pushes fluid into the interstitial space.5 In the nephrotic syndrome, massive proteinuria causes hypoalbuminemia to reduce plasma oncotic pressure and permits fluid extravasation.6,7 The scrotum and penis, because of their dependent position, loose areolar tissue, and rich vascular supply, become preferential sites for accumulation of edema in males with systemic fluid overload.2,4
The sequence of events usually proceeds from generalized edema to significant involvement of the genitalia, which suggests advanced disease in most cases. In both our cases, massive genital edema was developed despite medical management, reflecting the severity of the underlying systemic condition.1,3 Because the scrotal wall can accommodate large volumes of fluid, patients may develop dramatic enlargement that may entail marked functional impairment, such as difficulty with ambulation, sitting, and urination.2,4
Clinical Differentiation from Acute Surgical Conditions
The clinical challenge is identifying systemic genital oedema from acute surgical pathology that requires immediate intervention. Several features help differentiate these conditions.8
History: Systemic scrotal and penile edema typically develops gradually over days to weeks, though progression may accelerate. Patients have known underlying cardiac, renal, or hepatic disease and usually present with generalized edema . In contrast, testicular torsion presents with sudden-onset severe testicular pain,9 while Fournier’s gangrene features systemic toxicity, fever, and rapidly progressive necrosis.
Physical Examination: In systemic edema, the genital skin is tense and edematous but lacks the severe tenderness, crepitus, or necrotic changes characteristic of Fournier’s gangrene.4 The testes remain palpable and non-tender, unlike in torsion or severe epididymo-orchitis. Erythema may be present due to skin stretching but without the intense inflammation or bullae seen in necrotizing infections.2 Importantly, systemic edema is accompanied by edema elsewhere, particularly the lower extremities.1,8
Laboratory Findings: Systemic diseases causing genital edema demonstrate characteristic laboratory abnormalities: elevated BNP and evidence of volume overload in heart failure5; hypoalbuminemia and proteinuria in nephrotic syndrome6,7; or elevated liver enzymes and coagulopathy in cirrhosis.10 While mild leukocytosis may occur from systemic inflammation, the dramatic elevation and left shift seen in Fournier’s gangrene are absent.4
Role of Clinical Scoring Tools
Validated scoring systems such as the TWIST score have been developed to assist in risk stratification for testicular torsion in patients presenting with acute testicular pain.9 However, these tools are primarily designed for unilateral presentations with testicular pain and have limited applicability in cases of bilateral scrotal swelling associated with clear systemic disease and absence of testicular symptoms. In the context of known severe heart failure or nephrotic syndrome with generalized anasarca and bilateral symmetric genital edema, clinical judgment combined with focused ultrasound examination provides more appropriate diagnostic guidance than standardized torsion risk scores.
Role of Imaging
Scrotal ultrasound with color Doppler is the cornerstone of evaluation for acute scrotal swelling.8,9 In systemic scrotal and penile edema, characteristic findings include: diffuse thickening of the scrotal wall with subcutaneous fluid accumulation; increased vascularity in the scrotal wall (the “Fountain sign”)9; normal testicular parenchyma with homogeneous echotexture; symmetric bilateral arterial flow to both testes on Doppler; and absence of testicular masses, collections, or air.4,8
These findings effectively exclude testicular torsion (which shows decreased or absent testicular flow) and Fournier’s gangrene (which demonstrates subcutaneous air, fluid collections, and tissue necrosis).9 The ultrasound findings in our cases were definitive in establishing the diagnosis and avoiding unnecessary surgical exploration.
Point-of-Care Ultrasound in Clinical Practice
In the evaluation of suspected systemic scrotal edema, point-of-care ultrasound performed by the consulting urologist has several advantages. Bedside examination allows immediate assessment, directly correlates ultrasound findings with clinical presentation, and allows the rapid exclusion of surgical emergencies.8,9 When systemic etiology is highly suspected based on history and physical examination, focused bedside ultrasound by an experienced clinician is often sufficient to confirm diagnosis. The main goals are confirmation of normal testicular parenchyma and vascularity, ruling out acute conditions such as torsion or abscess formation, and confirmation of scrotal wall edema. In our cases, bedside ultrasound examination by the urology team provided definitive diagnostic information that allowed immediate reassurance and appropriate redirection of care to medical management. Formal imaging department studies with detailed Doppler interrogation remain indicated when bedside findings are equivocal or in which more complex pathology is suspected.
Management Considerations
Treatment of genital edema secondary to systemic disease focuses primarily on managing the underlying condition.11 However, several specific considerations apply:
Conservative Genital Management: Scrotal and penile elevation, supportive garments, and gentle skin care help prevent skin breakdown and provide symptomatic relief.8 Local measures do not address the underlying problem but improve patient comfort during medical optimization.
Treatment of Underlying Disease: In heart failure, optimization includes careful diuresis, afterload reduction, and management of cardiorenal syndrome . In nephrotic syndrome, aggressive diuretic therapy combined with albumin infusion may be necessary, along with immunosuppressive therapy to address the underlying glomerular disease.6,7 Sodium and fluid restriction are essential in both conditions.12
Complications: Patients with massive genital edema are at risk for several complications, including skin breakdown, infection, urinary retention from urethral compression, and impaired mobility.2,4 Severe genital oedema severely affects the quality of life and can lead to social isolation and depression.
Interventional Approaches: Such interventions as palliative scrotal centesis may be considered in extreme cases when conservative management and medical optimization do not adequately reduce scrotal edema, or in the case of severe functional impairment resulting from edema at the end of a disease process.2 This technique, described in palliative care literature for patients with terminal heart failure or cancer, involves needle drainage of fluid from the scrotal wall, providing rapid symptomatic relief. However, this should be reserved for specific circumstances and performed with appropriate patient selection and informed consent.
Clinical Implications and Learning Points
Our cases emphasize several important clinical lessons: (1) Systemic causes should be considered in patients presenting with genital swelling and known cardiac, renal, or hepatic disease; (2) Assessment should be thorough including an evaluation for generalized edema and appropriate laboratory testing1,4; (3) Imaging judiciously - ultrasound with Doppler is invaluable in confirming the diagnosis and excluding surgical emergencies8,9; (4) Attention should be directed to underlying disease - definite resolution of fluid overload requires the treatment of the systemic condition; (5) Multidisciplinary approach-close collaboration between urology, cardiology, nephrology, and other specialties optimizes patient care12; and (6) Patient education about the systemic nature of their condition.
Conclusion
Massive scrotal and penile edema secondary to systemic diseases such as heart failure and nephrotic syndrome represents an important but often underrecognized cause of acute genital swelling. While these patients frequently prompt urgent urological consultation due to concern for surgical emergencies, careful clinical assessment combined with ultrasound imaging can reliably distinguish systemic genital edema from conditions requiring surgical intervention. Recognition of this entity avoids fruitless surgical exploration and focuses attention appropriately on optimizing the management of the underlying systemic condition. Clinicians should be aware of this presentation, especially in patients with known cardiac, renal, or hepatic disease, for proper diagnosis and management. A multidisciplinary approach involving urology and the related medical subspecialty is thus optimal regarding patient care and outcomes.
Patient Consent
Written informed consent for publication of clinical details and photographs was obtained from both patients in accordance with institutional ethical guidelines.
Conflict of Interest
The authors declare no conflicts of interest.
Funding
This research received no specific grant from any funding agency.